Your Guide to Gum Disease and How to Manage Infections
12/01/2026 01:37
14/03/2026 14:06
When we think about oral health, we usually focus on our teeth. We care about how white they are, try to avoid cavities, and want straight smiles. But we often forget about the gums, which are the foundation that keeps our teeth in place.
Think of building a beautiful house on unstable ground. No matter how nice it looks, it will eventually fall apart if the base is weak. This is similar to gum health. Gum disease is the main reason adults lose teeth, but many people ignore it or think bleeding gums are not serious.
Healthy gums should not bleed. Seeing pink in the sink after brushing is your body’s way of warning you about an infection that needs attention. Gum disease often develops quietly, without pain, and can cause lasting damage before you notice any problems. This guide will explain how gum disease progresses, how it affects your overall health, and what treatments are available today.
The Culprit: Understanding the Biofilm
To manage the infection, we must understand its source. The mouth is a complex ecosystem. Bacteria constantly form a sticky, colorless film on teeth called plaque (biofilm). If this plaque is not removed by brushing and flossing, it hardens into tartar (calculus) within 48 hours. Tartar is like a coral reef for bacteria; it is rough and porous, allowing more bacteria to attach and multiply. You cannot brush tartar off; it requires professional removal.
Bacteria in tartar release toxins that irritate your gums and trigger your immune system. This ongoing battle causes the inflammation, redness, and tissue damage that we call gum disease.
Stage 1: Gingivitis (The Warning Shot)
Gingivitis is the first stage of gum disease, and it is the only stage that can be completely reversed.
The Signs: Gums become red, swollen, and bleed easily during brushing or flossing. Crucially, there is usually no pain.
The Pathology: The inflammation is limited to the soft tissues (gums). The bone supporting the teeth is still intact.
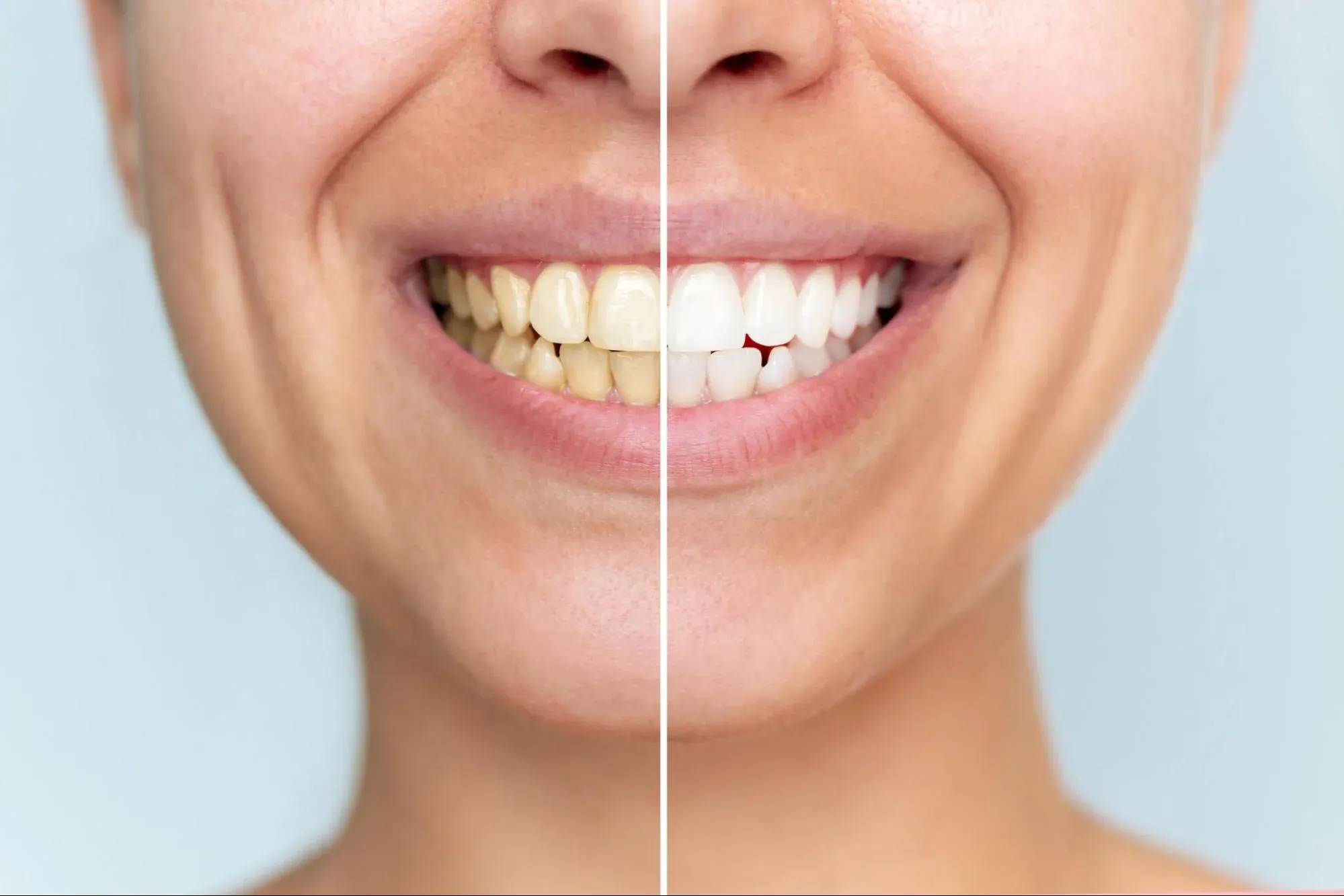
The Cure: Professional cleaning and improved home hygiene can eliminate the infection, and the gums will return to a healthy, pink, firm state.
Stage 2: Periodontitis (The Destruction Begins)
If gingivitis is not treated, the infection goes deeper, moving from the gums to the bone. This is when it becomes periodontitis.
The gums start to pull away from the teeth, creating spaces called periodontal pockets. These pockets trap food and bacteria that brushing cannot remove.
Bone Loss: The toxins produced by the bacteria, combined with the body's "overreacting" immune enzymes, begin to break down the bone and ligaments that hold the teeth in place.
The Consequence: This damage is irreversible. We can stop the progression, but we cannot easily grow back the lost bone.
Stage 3: Advanced Periodontitis (The End Game)
In the last stage, most of the bone that supports the teeth is gone.
Symptoms: Teeth become loose or shift positions. You might notice gaps forming between teeth that weren't there before. There may be a persistent bad taste in the mouth or active pus oozing from the gums.
If not treated quickly and thoroughly, the teeth will either fall out or need to be removed to stop the infection.
The Mouth-Body Connection
For decades, dentistry and medicine were treated as separate entities. Today, we know that the mouth is a mirror of the body. Periodontal disease is not just a localized problem; it is a systemic risk factor. The bacteria from infected gums can enter the bloodstream and travel to major organs, causing chronic inflammation throughout the body.
Heart Disease: Studies show that gum disease raises your risk of heart disease and stroke. The inflammation can make your arteries harder, a condition called atherosclerosis.
Diabetes: The link goes both ways. People with diabetes are more likely to get gum disease, and serious gum disease can make it harder to control blood sugar.
Pregnancy: Ongoing gum disease has been connected to early births and low birth weight in babies.
Respiratory Issues: Inhaling bacteria from the throat into the lungs can cause pneumonia, especially in the elderly.
Diagnosis: Charting the Landscape
Diagnosing gum disease requires more than a visual check. It requires Periodontal Charting. The dentist or periodontist uses a tiny ruler (probe) to measure the depth of the pockets around each tooth.
1-3 mm: Healthy.
4 mm: Early warning (Gingivitis).
5 mm and above: Periodontitis.
Dentists also use X-rays to see the bone levels and find bone loss between teeth that you cannot see or feel.
Non-Surgical Therapy: Scaling and Root Planing
The first line of defense against periodontitis is a "deep cleaning," technically known as Scaling and Root Planing (SRP). This is not a regular cleaning. It is usually performed under local anesthesia.
Scaling: Removing tartar from above and below the gum line.
Root Planing: This step smooths out the rough spots on the tooth roots. Bacteria have a harder time sticking to smooth surfaces, which helps the gums heal and reattach.
This treatment lowers the number of bacteria and makes the pockets smaller, often stopping the disease from getting worse without surgery.
Surgical Intervention: When Deep Cleaning Isn't Enough
In advanced cases where pockets are too deep to clean manually, periodontal surgery may be necessary.
Flap Surgery: The gum is lifted back to expose the roots for thorough cleaning and to reduce the pocket depth.
Bone Grafts: Placing material to encourage the body to regenerate lost bone.
Soft Tissue Grafts: Used to cover exposed roots due to gum recession.
Maintenance: A Lifelong Commitment
Here is the hard truth: Periodontitis cannot be "cured" like a cold; it can only be managed like diabetes. Once you have been diagnosed with periodontal disease, you remain a periodontal patient for life. The bacteria can return quickly if vigilance drops. This is why Supportive Periodontal Therapy (SPT) is critical. Instead of standard 6-month check-ups, periodontal patients typically need cleanings every 3 to 4 months. This frequency disrupts the bacterial lifecycle before it can cause new damage.
Prevention: The Power of Habit
The best way to deal with gum disease is to prevent it from starting in the first place.
Mechanical Cleaning: Brush your teeth twice a day, but do not skip flossing. Flossing is the only way to clean between your teeth, where gum disease often begins. If you have bigger gaps, interdental brushes work even better.
Lifestyle: Smoking is the biggest risk factor for gum disease. It reduces blood flow to your gums, hides signs of bleeding, and slows down healing. Quitting smoking is often the best thing you can do for your gum health.
Protecting the Foundation
Your gums play a key role in your oral health. They protect the bone, keep out bacteria, and support your smile. If you ignore bleeding gums or bad breath, you might miss early warning signs. By the time you feel pain, the damage may already be serious.
Managing gum disease is a team effort between you and your dental specialist. Finding problems early can turn a serious issue into something you can manage. If you need expert help with gum infections, the Periodontology Department at İstinye University Dental Hospital provides a full range of treatments, from basic care to advanced procedures, to help keep your smile healthy for years.