The Hinge of Health: Understanding Temporomandibular Joint (TMJ) Disorders
12/01/2026 01:58
30/03/2026 10:24
We eat, speak, yawn, and laugh. Most of us move our jaws more than 2,000 times a day, but we rarely think about how it all works until something goes wrong and it starts to hurt.
The Temporomandibular Joint (TMJ) is one of the body’s most complex and active joints. It connects your lower jaw to the temporal bone of your skull, just in front of your ears. Unlike the knee or elbow, which move like simple hinges, the TMJ lets your jaw move in many directions: up and down, side to side, and forward and backward. A soft cartilage disc cushions the bones to help everything move smoothly.
When this system stops working properly, it can cause a group of painful problems called Temporomandibular Disorders (TMD).
Millions of people live with TMD, which often causes ongoing pain that is hard to diagnose. Many see ear doctors for earaches or neurologists for headaches, but tests show nothing wrong. The real problem is often in the jaw’s complex movement. TMJ disorders can make life difficult, whether your jaw locks up or you hear clicking when you chew. This guide will help explain what causes the pain and walk you through treatment options, from managing stress to surgery.
The Warning Signs: It’s Not Just "Jaw Pain"
TMD can be tricky because its symptoms often spread to other areas, making it hard to know where the pain is really coming from.
-
The Noise: Clicking, popping, or a gritty "sandpaper" sound (crepitus) when opening the mouth. This usually indicates that the cushioning disc has slipped out of place.
-
You might feel a dull, aching pain in your face, jaw, neck, or shoulders. This pain often gets worse when you chew or first thing in the morning.
-
Ear Symptoms: Ringing in the ears (tinnitus), a feeling of fullness/stuffiness, or sharp earaches—despite a healthy ear canal.
-
Headaches: Frequent tension headaches or migraines, particularly in the temple area.
-
Limited Movement: Difficulty opening the mouth wide (e.g., trying to eat a burger) or the jaw getting "stuck" or locked in an open or closed position.
-
Tooth Sensitivity: Teeth feeling sensitive or loose without any signs of decay, caused by excessive pressure from clenching.
The Causes: A Perfect Storm
TMD rarely has just one cause. It usually happens because of a mix of physical factors, stress, and habits.
1. Bruxism (Teeth Grinding/Clenching): This is the main cause. Many people clench their jaws during the day, often while working, or grind their teeth at night. This puts a lot of pressure on the joint and tires out the muscles.
2. Stress: The TMJ is sometimes called the emotional center of the face. When we feel stressed, we often tighten our jaw muscles. Over time, this can cause tension, muscle spasms, and joint inflammation.
3. Malocclusion (Bad Bite): If your teeth don't fit together correctly, the jaw has to shift into an unnatural position every time you swallow or close your mouth. This constant micro-adjustment strains the joint ligaments.
4. Trauma: An injury to the jaw, whiplash from a car accident, or keeping your mouth open for a long dental procedure can all damage the joint.
5. Arthritis: Like your knees or hips, the TMJ can develop osteoarthritis from wear and tear or rheumatoid arthritis from inflammation.
The "Clicking" Mystery: Internal Derangement
The most common specific diagnosis is Internal Disc Derangement. Usually, the cartilage disc sits squarely on top of the jawbone (condyle) and travels with it. In displacement, the disc slips forward.
-
The "Click": When you open your mouth, the jawbone has to move over the slipped disc to get back in place. This movement causes the popping sound.
-
The Danger: If not treated, the disc can slip so far forward that it won’t move back. It blocks the jaw from opening fully, which is called a "Closed Lock" and needs urgent care
Diagnosis: Listening to the Joint
Diagnosis starts with a physical exam. The specialist will feel your jaw as you open and close it, listen for sounds, and check for any unusual movement. They’ll also measure how wide you can open your mouth.
-
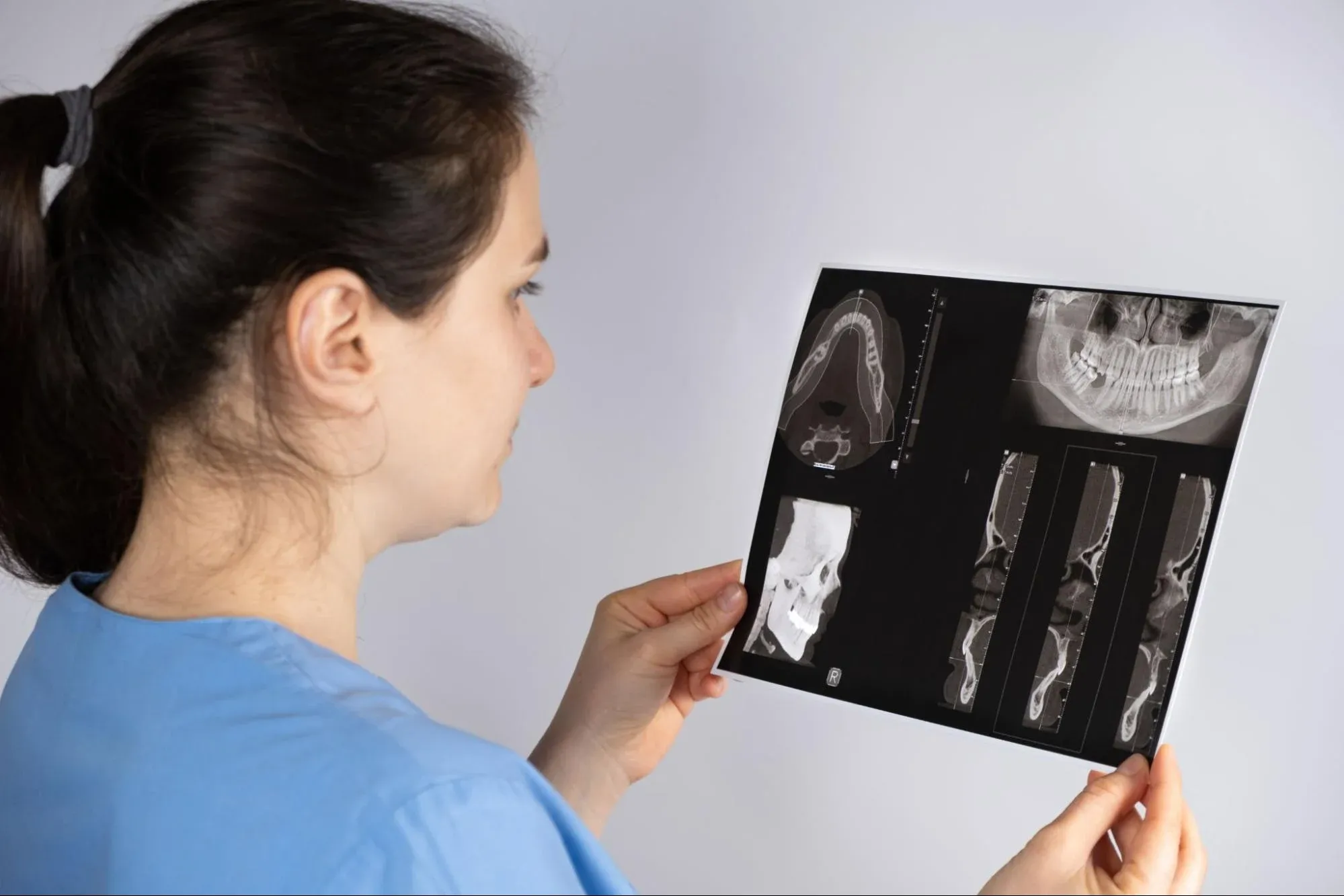
MRI: This is the best way to see soft tissues. It shows the exact position of the disc and if it’s torn.
-
CBCT (3D X-Ray): This scan checks the bones for problems like bone spurs, erosion, or arthritis in the jaw joint.
The Treatment Ladder: From Conservative to Complex
The main idea in treating TMJ is to start with simple steps. Most cases—about 90%—can be managed without surgery. Surgery is only considered when other treatments don’t work.
Step 1: The Conservative Phase (Lifestyle & Splints)
-
Occlusal Splints (Night Guards): These are a key part of treatment. They are custom-made hard acrylic devices worn over your teeth, usually at night. They help in three ways:
-
They keep your teeth from touching, which protects the enamel.
-
They slightly open your bite, taking pressure off the joint.
-
They help train your muscles to stop clenching.
-
Soft Diet: Give your jaw a break by avoiding chewy foods like bagels, gum, and hard nuts for a few weeks. This helps reduce inflammation.
-
Physical Therapy: Treatments may include ultrasound heat, jaw exercises to strengthen opening muscles, and massage to relax tight spots in your cheek muscles.
-
Medication: Anti-inflammatory drugs can help with pain, and muscle relaxants may stop nighttime spasms.
Step 2: Minimally Invasive Procedures. If simple treatments don’t work, the next step is to try these options.
-
Botox Injections: Botox is injected into the main chewing muscles. It weakens them just enough to stop intense grinding but doesn’t affect eating. This can bring a lot of relief for muscle-related TMJ pain.
-
Arthrocentesis (Joint Washing): This is a simple procedure done with local anesthesia or sedation. Two small needles are placed in the joint, and sterile fluid is used to wash out inflammation and break up small areas of scar tissue. Sometimes, hyaluronic acid is added to help lubricate the joint.
Step 3: Surgery. This is only for serious problems, like when the joint is fused, there are tumors, or there is severe arthritis.
-
Arthroscopy: Similar to knee surgery, a small camera and tools are inserted through a tiny cut to repair the disc or reshape the bone.
-
Open Joint Surgery: This is the most invasive option and involves making a cut near the ear to reach the joint directly.
-
Total Joint Replacement: In very severe cases, the joint can be replaced with a custom-made titanium part.
The Psychological Component
Since stress plays a big role in TMD, treatment often needs to address the whole person, not just the jaw. Methods like cognitive-behavioral therapy, meditation, and biofeedback can help. These techniques teach you to notice when you’re clenching your teeth and to relax your facial muscles.
Protecting Your Hinge
Living with TMJ pain can be exhausting. It makes eating a chore and talking painful. But it is not a condition you have to "just live with." The key is early intervention. Ignoring that clicking sound often leads to the more severe locking stage.
The first step is to realize that your jaw is part of a complex system of muscles and bones. You need a provider who understands not just teeth, but also muscles, nerves, and how the joint works.
For patients suffering from facial pain, clicking, or limited movement, the specialized TMJ Clinic at İstinye University Dental Hospital offers a multidisciplinary approach. Combining the expertise of prosthodontists, oral surgeons, and physiotherapists, we use advanced diagnostics such as MRI and dynamic jaw-tracking to pinpoint the root cause of your discomfort. From custom splint therapy to advanced arthroscopic solutions, we are dedicated to restoring the silent, smooth, and painless function of your jaw, allowing you to enjoy the simple pleasures of life again.